Overview
Thyroid cancer is a type of cancer that originates in the thyroid gland, a small, butterfly-shaped organ located at the base of the neck that plays a vital role in regulating metabolism, heart rate, body temperature and energy levels. Although thyroid cancer is considered less common compared to many other cancers, its incidence has increased steadily over the past few decades. This rise is largely attributed to advancements in diagnostic imaging, improved screening methods and greater public awareness, which have enabled earlier and more accurate detection. When identified at an early stage, thyroid cancer is highly treatable, with excellent survival rates and favorable long-term outcomes. This makes thyroid cancer awareness, early diagnosis and timely medical intervention critically important.
In this comprehensive guide, we explore the early signs and symptoms, underlying causes and risk factors, diagnostic methods, modern treatment options, preventive strategies and quality-of-life considerations for survivors. Whether you are a patient, caregiver or health-conscious individual, this article aims to provide essential, life-saving knowledge.
What Is Thyroid Cancer?
The thyroid gland produces hormones that regulate metabolism, heart rate, body temperature and energy levels. When cells in the thyroid begin to grow abnormally, they can form a tumor. If these tumor cells become malignant and invade surrounding tissues or spread to other body parts, this is known as thyroid cancer.
Unlike many other cancers, thyroid cancer often grows slowly and may remain asymptomatic in early stages. This is why awareness and regular checkups are essential, especially for individuals with risk factors.
Types of Thyroid Cancer
Thyroid cancer is divided into several subtypes based on the appearance of cells under a microscope-
✓Papillary Thyroid Cancer
- Most common type (about 80% of cases).
- Grows slowly and often remains localised.
- Highly treatable with excellent long-term survival.
✓Follicular Thyroid Cancer
- Second most common type.
- Tends to occur in older adults.
- Treatment outcomes are also generally positive.
✓Medullary Thyroid Cancer
- Arises from C-cells that produce calcitonin.
- May be hereditary or sporadic.
- Requires specialised monitoring and treatment.
✓Anaplastic Thyroid Cancer
- Rare but aggressive.
- Often diagnosed at advanced stages.
- Treatment focuses on controlling growth and symptoms.
Understanding the subtype is critical in planning treatment and determining prognosis.
Why Awareness Matters
Thyroid cancer is highly treatable when diagnosed early, but delayed detection can allow the disease to spread beyond the thyroid gland, making treatment more complex and outcomes less favorable. Early awareness helps individuals recognise warning signs such as neck lumps, voice changes or difficulty swallowing and seek timely medical evaluation. Prompt diagnosis significantly improves survival rates and reduces the need for aggressive treatments.
Many thyroid cancers develop silently and are often discovered incidentally during imaging tests performed for unrelated medical conditions. This highlights the importance of routine physical examinations and appropriate diagnostic imaging, especially for individuals with underlying risk factors.
Increased awareness enables early detection, timely treatment and better long-term quality of life for thyroid cancer patients.
Early Signs and Symptoms-
Thyroid cancer often has subtle early signs, but any persistent or unusual symptom in the neck region should be evaluated by a healthcare professional.
Common Early Warning Signs-
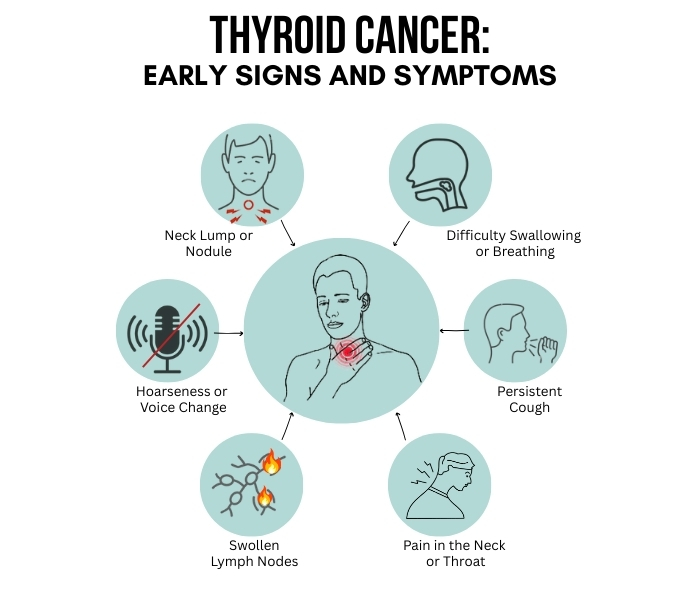
☑ Neck Lump or Nodule
A painless lump or swelling in the front part of the neck is the most common early sign of thyroid cancer. These nodules can vary in size and may initially be too small to feel.
☑ Difficulty Swallowing or Breathing
As a thyroid tumor grows, it can press against the esophagus or windpipe (trachea), causing discomfort with swallowing or breathing.
☑ Hoarseness or Voice Changes
Persistent hoarseness or changes in voice quality can occur if the tumor affects the recurrent laryngeal nerve, which controls vocal cords.
☑ Persistent Cough
A new cough that does not go away and is not related to a cold or respiratory infection warrants further evaluation.
☑ Swollen Lymph Nodes
Enlargement of lymph nodes in the neck, especially on one side, may suggest cancer spread.
☑ Pain in the Neck or Throat
While not as common, some patients experience discomfort or pain in the front of the neck.
Importantly, these symptoms can also be caused by non-cancerous conditions. However, early evaluation ensures that if cancer is present, it is treated when most manageable.
Causes and Risk Factors
The exact cause of thyroid cancer is not known, but several factors increase the likelihood of developing the disease-
1. Radiation Exposure
Exposure, especially during childhood, is one of the strongest risk factors for thyroid cancer. Radiation therapy to the head, neck, or chest can damage thyroid cells and trigger abnormal growth years later. Environmental or occupational radiation exposure may also increase risk.
2. Gender and Age
Thyroid cancer occurs two to three times more often in women than in men, likely due to hormonal influences. It is most commonly diagnosed between the ages of 30 and 60, though it can occur at any age. Age and gender together play an important role in risk assessment.
3. Family History and Genetic Syndromes
Having a close family member with thyroid cancer increases the likelihood of developing the disease. Certain inherited genetic conditions, such as familial medullary thyroid carcinoma and MEN syndromes, are strongly linked to thyroid cancer. Genetic screening enables early detection in high-risk individuals.
4. Iodine Deficiency or Excess
It is essential for healthy thyroid function and imbalance can affect thyroid cells. Iodine deficiency is associated with a higher risk of follicular thyroid cancer in some regions. Excess iodine intake may also disrupt thyroid hormone regulation in susceptible individuals.
5. Thyroid Disorders
Existing thyroid conditions such as goiter, thyroid nodules and chronic thyroiditis may increase cancer risk. Long-term inflammation or abnormal thyroid activity can lead to cellular changes over time. Regular monitoring of thyroid disorders is essential for early detection.
6. Lifestyle and Environmental Factors
Environmental pollutants and endocrine-disrupting chemicals may influence thyroid health. Obesity, poor dietary habits and a sedentary lifestyle are being studied as potential contributors. Healthy lifestyle choices may help reduce overall thyroid cancer risk.
Understanding these risk factors helps in early detection strategies, especially for high-risk individuals.

Diagnosis: How Thyroid Cancer Is Identified
When a thyroid abnormality is suspected either due to symptoms, physical findings or incidental imaging results a systematic and multi-step diagnostic approach is used to confirm or rule out thyroid cancer. Accurate diagnosis not only determines whether a thyroid nodule is malignant, but also helps identify the cancer type, stage and the most effective treatment strategy. Physicians may recommend one or more of the following diagnostic evaluations-
1. Physical Examination- The doctor examines the neck to check for lumps, swelling or abnormal enlargement of the thyroid gland. Nearby lymph nodes are also assessed for signs of possible cancer spread.
2. Thyroid Function Tests- Blood tests measure thyroid hormones (T3, T4) and thyroid-stimulating hormone (TSH) to evaluate how well the thyroid is functioning. While these tests do not confirm cancer, they help identify underlying thyroid disorders.
3. Ultrasound Imaging- Ultrasound uses sound waves to create detailed images of the thyroid gland and detect nodules. It helps assess nodule size, structure and features that may suggest malignancy.
4. Fine Needle Aspiration Biopsy (FNAB)- A thin needle is used to collect a small sample of thyroid cells for microscopic examination. This test is the most accurate way to determine whether a thyroid nodule is cancerous.
5. Genetic and Molecular Testing- Specialised tests identify genetic mutations linked to thyroid cancer, especially in medullary and high-risk cases. These results help guide treatment decisions and assess hereditary risk.
6. CT, MRI, or Nuclear Scans- Advanced imaging is used to evaluate tumor size, spread to lymph nodes or involvement of nearby structures. These scans are typically recommended for advanced or complex thyroid cancer cases.
Treatment Options for Thyroid Cancer
Thanks to advanced medical techniques, most thyroid cancers are highly treatable. Treatment choice depends on the type, stage, patient age, overall health and genetic factors.
☑ Surgery
Thyroidectomy – Removing all or part of the thyroid gland is the most common treatment.
Types include-
- Lobectomy– Removing one lobe of the thyroid.
- Total thyroidectomy– Removing the entire gland.
- Neck dissection– Removing nearby lymph nodes if cancer has spread.
Surgery is often curative, especially in early stages.
☑ Radioactive Iodine Therapy
Used after surgery to destroy remaining thyroid tissue or microscopic cancer cells. It’s particularly useful in papillary and follicular thyroid cancers.
☑ Hormone Therapy
Thyroid hormone replacement (levothyroxine) is given to-
- Replace hormones the thyroid no longer makes
- Suppress TSH to reduce the chance of recurrence
☑ Targeted Therapy
For certain advanced or aggressive cancers, drugs that target specific genetic mutations (e.g., RET, BRAF) can slow cancer growth.
☑ External Beam Radiation
Used less commonly, but helpful in cases where surgery isn’t feasible or cancer recurs.
☑ Chemotherapy
Rarely used in thyroid cancer, reserved for aggressive or anaplastic types.
Survival Rates and Prognosis
Thyroid cancer typically has excellent survival outcomes, especially when detected early-
- Papillary and follicular cancershave 10-year survival rates above 90–95%.
- Medullary thyroid cancerhas a good prognosis when localised.
- Anaplastic thyroid canceris more challenging, requiring aggressive multimodal therapy.
Prognosis depends on the cancer type, stage, patient age and response to treatment.
Living With Thyroid Cancer: What to Expect
Post-Treatment Care
After treatment, patients may need:
- Regular physical exams and imaging
- Blood tests to monitor hormone levels and detect recurrence
- Lifelong thyroid hormone replacement
Managing Side Effects
Hormone therapy may lead to symptoms such as-
- Weight changes
- Fatigue
- Mood fluctuations
- Temperature intolerance
These are usually manageable with dose adjustments and clinical follow-up.
Emotional and Psychological Support
A cancer diagnosis can be emotionally challenging. Support groups, counseling and survivorship programs can improve mental well-being.
Preventive Strategies and Screening
There’s no definitive way to prevent thyroid cancer, but steps that may lower risk include-
- Avoiding unnecessary radiation exposure
- Regular medical checkups, especially if you have risk factors
- Managing thyroid disorders early
- Staying aware of neck changes
People with strong family histories or known genetic syndromes may benefit from genetic counseling and targeted monitoring.
Thyroid Cancer in Special Populations
Children and Adolescents
Thyroid cancer is rare in children but often more aggressive. Early detection and specialist care are critical.
Pregnancy and Thyroid Cancer
Management requires balance between maternal and fetal health. Treatment planning is individualised based on cancer stage and pregnancy timing.
Conclusion: Awareness Saves Lives
Thyroid cancer may be silent in its early stages, but awareness, early detection and timely intervention dramatically improve outcomes. With modern diagnostic tools and highly effective therapies, many individuals with thyroid cancer live long, healthy lives post-treatment.
Key takeaways-
- Watch for neck lumps, changes in swallowing or voice and persistent symptoms.
- Understand personal risk factors, especially family history and past radiation exposure.
- Seek medical evaluation earlyif symptoms persist.
- Follow through with recommended diagnostic tests and treatments.
- Embrace ongoing surveillance and follow-up care after treatment.
Knowledge is empowerment and in the case of thyroid cancer, awareness can be truly life-saving.
Contact Medikaya Healthcare for Thyroid Cancer Support in India
If you are seeking verified medical information, private hospital options, treatment cost guidance, or international patient support for kidney treatment in India, our medical coordination team is here to assist you with complete confidentiality and professional care.
Medikaya Healthcare provides end-to-end patient support, including hospital selection, doctor consultations, medical visa assistance, treatment coordination, and post-treatment follow-up.
📞 WhatsApp & Call: +91 9717998697
📧 Email: info@medikayahealthcare.com
🌐 Website: www.medikayahealthcare.com
Follow us on:
LinkedIn | Instagram | Facebook | Twitter
Our team will respond promptly with verified medical guidance and personalised assistance.

